Page 36 - SPEMD_59-1
P. 36
28 rev port estomatol med dent cir maxilofac. 2018;59(1):24-29
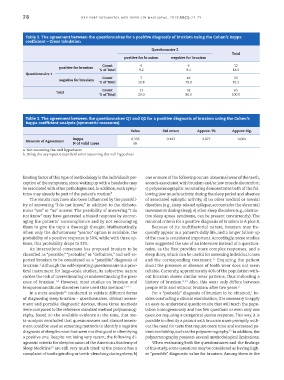
Table 2. The agreement between the questionnaires for a positive diagnosis of bruxism using the Cohen’s kappa
coefficient – Cross tabulation
Questionnaire 2
Total
positive for bruxism negative for bruxism
Count 6 6 12
positive for bruxism
% of Total 9.2 9.2 18.5
Questionnaire 1
Count 7 46 53
negative for bruxism
% of Total 10.8 70.8 81.5
Count 13 52 65
Total
% of Total 20.0 80.0 100.0
Table 3. The agreement between the questionnaires Q1 and Q2 for a positive diagnosis of bruxism using the Cohen’s
kappa coefficient analysis (symmetric measures)
Value Std errora Approx. Tb Approx Sig.
kappa 0.356 0.143 2.877 0.004
Measure of Agreement
N of valid cases 65
a. Not assuming the null hypothesis
b. Using the asymptotic standard error assuming the null hypothesi
limiting factor of this type of methodology is the individual’s per- one or more of the following occurs: abnormal wear of the teeth,
ception of the symptoms, since waking up with a headache may sounds associated with bruxism and/or jaw muscle discomfort;
be associated with other pathologies and, in addition, such symp- c) polysomnographic monitoring demonstrates both of the fol-
toms may already be part of the patient’s routine. 8 lowing: jaw muscle activity during the sleep period and absence
The results may have also been influenced by the possibil- of associated epileptic activity; d) no other medical or mental
ity of answering “I do not know,” in addition to the dichoto- disorders (e.g., sleep-related epilepsy, accounts for the abnormal
mous “yes” or “no” answer. The possibility of answering “I do movements during sleep); e) other sleep disorders (e.g., obstruc-
not know” may have generated a biased response by encour- tive sleep apnea syndrome, can be present concurrently). The
aging the patients’ noncompliance and by not encouraging minimal criteria for a positive diagnosis of bruxism is A plus B.
them to give the topic a thorough thought. Mathematically, Because of its multifactorial nature, bruxism may fre-
when only the dichotomous “yes/no” option is available, the quently appear in a patient’s daily life, and a longer follow-up
probability of a positive response is 50%, while with three op- of the case is considered important. Accordingly, some studies
tions, this probability drops to 33%. have suggested the use of an interview instead of a question-
An international consensus has proposed bruxism to be naire, as the first provides more complex responses, and a
classified as “possible,” “probable,” or “definitive,” and self-re- sleep diary, which can be useful for assessing individual cases
17
ported bruxism to be considered as a “possible” diagnosis of and the corresponding treatment. Enquiring the patient
1
bruxism. Although the self-reporting questionnaire is a prac- about the presence or absence of tooth wear does not seem
tical instrument for large-scale studies, its subjective nature reliable. Currently, approximately 40% of the population with-
carries the risk of overestimating or underestimating the pres- out bruxism shows similar wear patterns, thus indicating a
ence of bruxism. 1,4 However, most studies on bruxism and history of bruxism. 8,11 Also, this wear only differs between
temporomandibular disorders have used this method. 15-17 people with and without bruxism after two years. 2
18
1
In a meta-analysis conducted to validate different forms For a “probable” diagnosis of bruxism to be obtained, be-
of diagnosing sleep bruxism – questionnaires, clinical assess- sides conducting a clinical examination, it is necessary to apply
ment and portable diagnostic devices, these three methods an easy-to-understand questionnaire that will reach the popu-
were compared to the reference standard method polysomnog- lation homogeneously and has few questions or even only one
raphy. Based on the available evidence at the time, that me- question requiring a categorical yes/no response. This way, it is
ta-analysis concluded that questionnaires and clinical assess- possible to identify a patient with bruxism more promptly with-
ment could be used as screening methods to identify a negative out the need for tests that require more time and increased pa-
15
diagnosis of sleep bruxism but were not that good in identifying tient availability, such as the polysomnography. In addition, the
a positive one. Despite not being very recent, the following di- polysomnography presents several methodological limitations.
agnostic criteria for sleep bruxism of the American Academy of When evaluating both the questionnaires and the findings
Sleep Medicine are still very much cited: a) the patient has a of this study, some questions may be considered as having high-
19
complaint of tooth-grinding or tooth-clenching during sleep; b) er “possible” diagnostic value for bruxism. Among them is the