Page 62 - SPEMD_61-3
P. 62
152 rev port estomatol med dent cir maxilofac. 2020;61(3):148-153
2
and [5] multiple compartments. Thus, the present case is
highly predictive of GOC, as all aforementioned characteristics
were present, in addition to the presence of ciliate and mucous
cells.
GOC may exhibit morphological similarities to other cystic
jaw lesions, such as dentigerous cysts displaying metaplastic
changes, ciliated surgical cysts, lateral periodontal cysts, root
cysts, residual cysts with mucous metaplasia, and botryoid
8,2
odontogenic cysts. The low -grade variant of the central mu-
coepidermoid carcinoma should also be considered a differ-
ential GOC diagnosis since these lesions share certain histo-
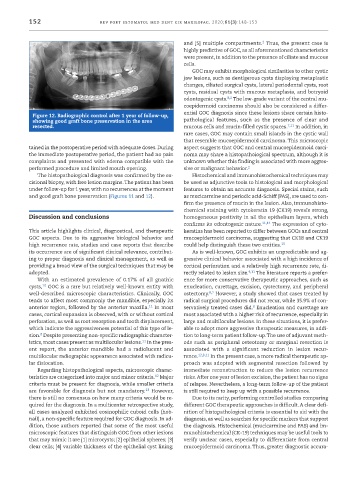
Figure 12. Radiographic control after 1 year of follow -up,
showing good graft bone preservation in the area pathological features, such as the presence of clear and
resected. mucous cells and mucin -filled cystic spaces. 7,11 In addition, in
rare cases, GOC may contain small islands in the cystic wall
that resemble mucoepidermoid carcinoma. This microscopic
tained in the postoperative period with adequate doses. During aspect suggests that GOC and central mucoepidermoid carci-
the immediate postoperative period, the patient had no pain noma may share a histopathological spectrum, although it is
complaints and presented with edema compatible with the unknown whether this finding is associated with more aggres-
performed procedure and limited mouth opening. sive or malignant behavior. 2
The histopathological diagnosis was confirmed by the ex- Histochemical and immunohistochemical techniques may
cisional biopsy, with free lesion margins. The patient has been be used as adjunctive tools to histological and morphological
under follow -up for 1 year, with no recurrences at the moment features to obtain an accurate diagnosis. Special stains, such
and good graft bone preservation (Figures 11 and 12). as mucicarmine and periodic acid -Schiff (PAS), are used to con-
firm the presence of mucin in the lesion. Also, immunohisto-
chemical staining with cytokeratin 19 (CK19) reveals strong,
Discussion and conclusions homogeneous positivity in all the epithelium layers, which
confirms its odontogenic nature. 11,14 The expression of cyto-
This article highlights clinical, diagnostical, and therapeutic keratins has been reported to differ between GOCs and central
GOC aspects. Due to its aggressive biological behavior and mucoepidermoid carcinoma, suggesting that CK18 and CK19
high recurrence rate, studies and case reports that describe could help distinguish these two entities. 15
its occurrence are of significant clinical relevance, contribut- As is well -known, GOC exhibits an unpredictable and ag-
ing to proper diagnosis and clinical management, as well as gressive clinical behavior associated with a high incidence of
providing a broad view of the surgical techniques that may be cortical perforation and a relatively high recurrence rate, di-
adopted. rectly related to lesion size. 4,11 The literature reports a prefer-
With an estimated prevalence of 0.17% of all gnathic ence for more conservative therapeutic approaches, such as
10
cysts, GOC is a rare but relatively well -known entity with enucleation, curettage, excision, cystectomy, and peripheral
8,2
well -described microscopic characteristics. Clinically, GOC ostectomy. However, a study showed that cases treated by
tends to affect most commonly the mandible, especially its radical surgical procedures did not recur, while 35.9% of con-
8
11
anterior region, followed by the anterior maxilla. In most servatively treated cases did. Enucleation and curettage are
cases, cortical expansion is observed, with or without cortical most associated with a higher risk of recurrence, especially in
perforation, as well as root resorption and tooth displacement, large and multilocular lesions. In these situations, it is prefer-
which indicate the aggressiveness potential of this type of le- able to adopt more aggressive therapeutic measures, in addi-
8
sion. Despite presenting non -specific radiographic character- tion to long -term patient follow -up. The use of adjuvant meth-
istics, most cases present as multilocular lesions. In the pres- ods such as peripheral osteotomy or marginal resection is
11
ent report, the anterior mandible had a radiolucent and associated with a significant reduction in lesion recur-
multilocular radiographic appearance associated with radicu- rence. 12,8,11 In the present case, a more radical therapeutic ap-
lar dislocation. proach was adopted with segmental resection followed by
Regarding histopathological aspects, microscopic charac- immediate reconstruction to reduce the lesion recurrence
12
teristics are categorized into major and minor criteria. Major risks. After one year of lesion excision, the patient has no signs
criteria must be present for diagnosis, while smaller criteria of relapse. Nevertheless, a long -term follow -up of the patient
13
are favorable for diagnosis but not mandatory. However, is still required to keep up with a possible recurrence.
there is still no consensus on how many criteria would be re- Due to its rarity, performing controlled studies comparing
quired for the diagnosis. In a multicenter retrospective study, different GOC therapeutic approaches is difficult. A clear defi-
all cases analyzed exhibited eosinophilic cuboid cells (hob- nition of histopathological criteria is essential to aid with the
nail), a non -specific feature required for GOC diagnosis. In ad- diagnosis, as well as searches for specific markers that support
dition, those authors reported that some of the most useful the diagnosis. Histochemical (mucicarmine and PAS) and im-
microscopic features that distinguish GOC from other lesions munohistochemical (CK -19) techniques may be useful tools to
that may mimic it are [1] microcysts; [2] epithelial spheres; [3] verify unclear cases, especially to differentiate from central
clear cells; [4] variable thickness of the epithelial cyst lining; mucoepidermoid carcinoma. Thus, greater diagnostic accura-